A breech birth occurs when a baby is born bottom first instead of head first. Around 3-5% of pregnant women at term (37–40 weeks pregnant) will have a breech baby.
Most babies in the breech position are born by a caesarean section because it is seen as safer than being born vaginally.
When a baby is born bottom first there is more risk that the birth will not be straight forward and that the baby could be harmed.For example, when the baby’s head is passing through the mother’s pelvis the umbilical cord can get squashed which stops the baby’s oxygen supply. Due to this and other risks, babies in breech position are usually born by a planned caesarean section in developed countries.
Caesarean section reduces the risk of harm or death for the baby but does increase risk of harm to the mother compared with a vaginal delivery. It is best if the baby is in a head down position so that they can be born vaginally with less risk of harm to both mother and baby. The next section is looking at External Cephalic Version or ECV which is a method that can help the baby turn from a breech position to a head down position.
Vaginal birth of a breech baby has its risks but caesarean sections are not always available or possible, a mother might arrive in hospital at a late stage of her labour or may choose not to have a caesarean section. In these cases, it is important that the clinical skills needed to deliver breech babies are not lost so that mothers and babies are as safe as possible. Compared with developed countries, planned caesarean sections have not produced as good results in developing countries – it is suggested that this is due to more breech vaginal deliveries being performed by experienced, skilled practitioners in these settings.
Turning the baby, technically known as external cephalic version (ECV), is when the baby is turned by gently pressing the mother’s abdomen to push the baby from a bottom first position, to a head first position. ECV does not always work, but it does improve the mother’s chances of giving birth to her baby vaginally and avoiding a cesarean section. The World Health Organisation recommends that women should have a planned cesarean section only if an ECV has been tried and did not work.
Women who have an ECV when they are 36–40 weeks pregnant are more likely to have a vaginal delivery and less likely to have a cesarean section than those who do not have an ECV. Turning the baby before this time makes a head first birth more likely but ECV before the due date can increase the risk of early or premature birth which can cause problems to the baby.
There are treatments that can be used which might affect the success of an ECV. Drugs called beta-stimulant tocolytics help the woman’s muscles to relax so that the pressure during the ECV does not have to be so great. Giving the woman these drugs before the ECV improves the chances of her having a vaginal delivery because the baby is more likely to turn and stay head down. Other treatments such as using sound, pain relief drugs such as epidural, increasing the fluid around the baby and increasing the amount of fluids to the woman before the ECV could all effect its success but there is not enough research to make this clear.
Turning techniques mothers can do at home are referred to Spontaneous Cephalic Version (SCV), this is when the baby can turn without any medical assistance. Some of these techniques include; a knee to chest position, the breech tilt and moxibustion, these can be performed after the mother is 34 weeks pregnant. Although there is not a lot of evidence to support how well these techniques work, it has worked for some mothers.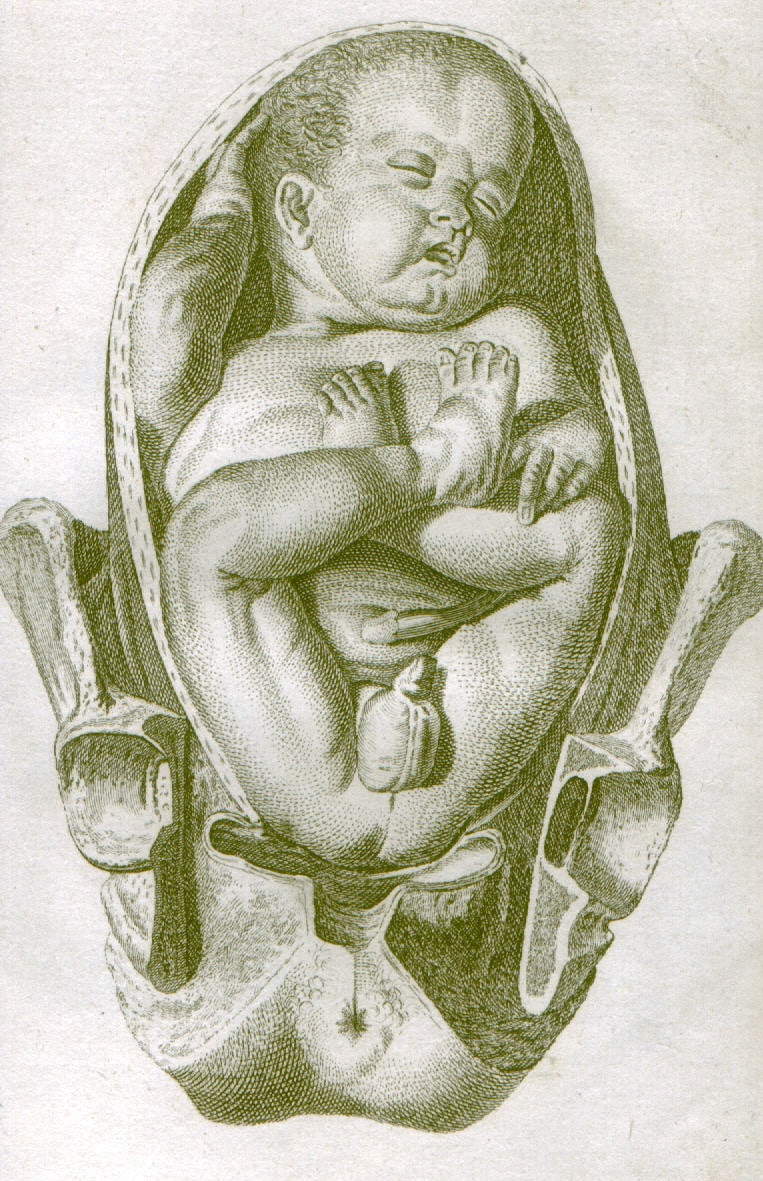
Breech birth. (2016, September 24). In Wikipedia, The Free Encyclopedia. Retrieved 21:03, September 24, 2016, from https://en.wikipedia.org/w/index.php?title=Breech_birth&oldid=741017026
